Functions of the Respiratory Portion
The respiratory portion consists of respiratory bronchioles, alveolar ducts, alveolar sacs and alveoli. It is hard to investigate the organisation of these structures in sections, because when the lungs are removed, they collapse. Basically the respiratory system consists of a branching set of air spaces, which are in close proximity to pulmonary capillaries. The air space is exchanged around 10 to 15 times a minute. The air spaces are within 0.2µm of the blood, which is a very thin barrier to diffusion. This arrangement means there is a fast efficient transfer of oxygen and carbon dioxide between the blood and the air, the major function of the respiratory portion.
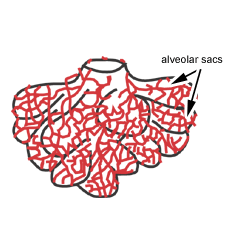 The terminal bronchioles branch to give rise to respiratory bronchioles, which lead to alveolar ducts, alveolar sacs and alveoli.
The terminal bronchioles branch to give rise to respiratory bronchioles, which lead to alveolar ducts, alveolar sacs and alveoli.
This diagram shows a diagram of an alveolar sac, showing how the organisation of the alveoli, and the network of blood capillaries that surround the alveoli (in red). These capillaries are derived from the pulmonary arterioles.
Gaseous exchange between the blood and air takes place in the alveoli, but the detailed structure of the alveolar walls cannot be resolved with the light microscope.
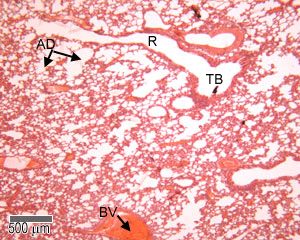
This shows a photograph of a section of adult lung. You should be able to recognise the terminal bronchioles, respiratory bronchioles, alveolar ducts and alveolar sacs, together with blood vessels.
The respiratory bronchioles have single alveoli off their walls. The epithelium is ciliated cuboidal epithelium and contains some secretory cells called clara cells.
The respiratory bronchioles lead into alveolar ducts, (which are surrounded by smooth muscle, elastin and collagen), which lead into the alveolar sacs. These have several alveoli, surrounded by blood vessels - from the pulmonary system.
This is a cross section through the lung, showing alveolar sacs, and alveoli
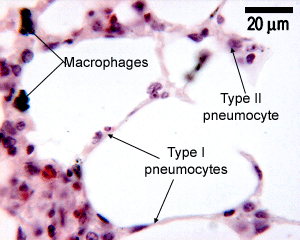
This is a section through the lung at higher magnification, showing the thin type I pneumocytes, and the type II pneumocytes. Notice how the type II pneumocytes look shorter and fatter, and have paler staining nuclei. Macrophages are also present.
Alveoli
The epithelium of the alveoli, contains two main types of cells:
1. type I pneumocytes: large flattened cells - (95% of the total alveolar area) which present a very thin diffusion barrier for gases. They are connected to each other by tight junctions.
2. type II pneumocytes (making up 5% of the total alveolar area, but 60% of total number of cells). These cells secrete 'surfactant' which decreases the surface tension between the thin alveolar walls, and stops alveoli collapsing when you breathe out. these cells are connected to the epithelium and other constituent cells by tight junctions.
The surfactant is made up of phospholipids, combined with carbohydrate and protein, which are released by exocytosis, and form a tubular lattice of lipoprotein. The surfactant overcomes surface tension, where the two alveolar surfaces come together. Otherwise the two thin alveolar walls might stick together, rather like a balloon that is deflated, after being inflated.
Macrophages are important for ingesting bacteria and particles, and arise from monocytes, which have escaped from the blood capillaries.
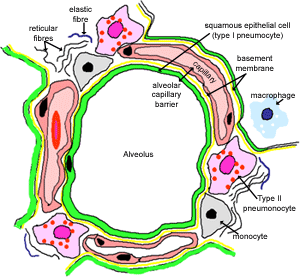
This diagram shows the main constituents of alveolus, and the interalveolar wall. The thickness of the alveolar-capillary barrier varies from 0.2 to 2.5 µm. The wall of the capillary endothelial cell is fused to that of the alveolar cell with only a very thin basement membrane between these two cells. This produces a very narrow gap across which oxygen and carbon dioxide can rapidly diffuse.
Now take a look through the lung for yourself, and try to recognise as much as you can.
 The terminal bronchioles branch to give rise to respiratory bronchioles, which lead to alveolar ducts, alveolar sacs and alveoli.
The terminal bronchioles branch to give rise to respiratory bronchioles, which lead to alveolar ducts, alveolar sacs and alveoli.

