Ovarian follicles
This image shows primordial follicles.
Can you identify them, together with the tunica albuginea - the
thick collagenous capsule, together with the germinal epithelium
that covers it, and the connective tissue in the cortex of the ovary,
known as the stroma.
Primordial follicle

Primordial germ cells migrate into the developing gonad early in
embryogenesis, and differentiate into oogonia. These oogonia proliferate
by mitosis. Some of these enlarge and develop into larger cells
called primary oocytes and enter the first meiotic division on the
pathway to making gametes by meiosis.
This happens between 3 and 8 months of gestation in the human embryo.
These 'primary' oocytes become arrested in prophase of the first
meiotic division until the female becomes sexually mature.
At sexual maturity, a small number of primary oocytes (20-50) mature
each month and complete the fist meiotic division to become secondary
oocytes, under the influence of follicle stimulating hormone.
The oocytes synthesise a coat and cortical granules - this glycoprotein
coat is called the 'zona pellucida'. They also accumulate ribosomes,
yolk, glycogen, lipid and the mRNA that will be used later on after
fertilisation to direct early development of the embryo.
After a second mitotic division, ova are formed.
In primordial follicles, the oocyte is arrested in the last stage
of prophase (known as dictyotene). At this stage, it is surrounded
by a single layer of flattened ovarian follicular epithelial
cells. (These cells are also known as granulosa cells).
They are small, and usually found close to the outer edge of the cortex.
The image shown here, has a primordial follicle. Can you identify
it, and the primary oocyte, follicular
cells, theca interna and zona pelucida?
Primary follicle
When the primordial follicle is stimulated, it becomes a primary
follicle. The oocyte enlarges, and the follicular cells
divide. A follicle that has two layers of follicular cells is called
a primary follicle. These cells continue to hypertrophy and proliferate
to form many layers surrounding the oocyte. Eventually these cells
become known as 'granulosa' cells. The granulosa cells will secrete
progesterone after ovulation.

A thick glycoprotein layer develops between the oocyte and the
zona granulosa, called the zona pellucida.
Finally, the stroma around the follicle develops
to form a capsule like 'theca'. (Theca is greek for 'box'). Only
one of the maturing follicles completes the maturation process each
month. The rest degenerate into atretic follicles.
Follicular maturation takes about 3 months.
This is an image of a secondary follicle. Can you identify the oocyte, theca interna
and externa, follicular cells,
and follicular fluid?
Secondary Follicle

The primary follicle develops into a secondary follicle.The
secondary follicles look very similar to primary follicles, except
that they are larger, there are more follicular cells, and there
are small accumulations of fluid in the intracellular spaces called
follicular fluid (nutritive fluid for the oocyte).
These gradually coalesce to form an antrum.
The surrounding granulosa cells is called the cumulus oophorus
(greek for 'egg bearing heap').
The surrounding theca differentiates into two layers: the Theca
interna (rounded cells that secrete androgens and follicular
fluid) and a more fibrous Theca externa
- spindle shaped cells. The androgens are converted into oestrogen
by the granulosa cells.
Can you identify the antrum, membrana granulosa, cumulus
oophorus, theca externa and theca interna
in this image of a Graafian follicle?
Graffian follicle.
The secondary follicle develops into a Graffian follicle.
The first meiotic division is now completed, and the oocyte is
now a secondary oocyte, and starts its second meiotic division.
After the first meiotic division, most of the cytoplasm goes into
one of the two daughter cells. The other becomes the polar body
(hard to see).
The folicular fluid fills a single space, called the antrum,
which is surrounded by the follicular cells - called the membrana
granulosa. The granulosa cells that surround the oocyte,
and project into the antrum are called as the cumulus oophorus.
There is a basement membrane between the granulosa cells and the
theca interna. The fibrous theca externa
merges with the surrounding stroma.
The oocyte, zona pellucida and
the follicular cells surrounding the ooctye (known as the corona
radiata) are all expelled at ovulation, and enter the
fallopian tube.
Once released, the oocyte begins its second meiotic division, as
far as metaphase II. Division only carries on if the ovum is fertilised.
Corpus Luteum
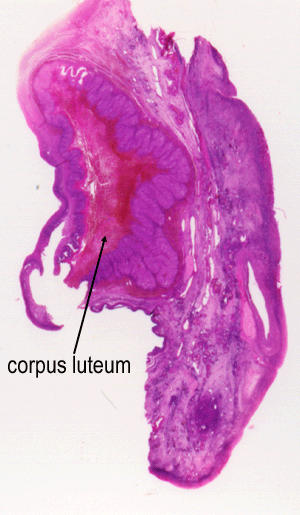
After ovulation, the ruptured follicle collapses and fills with
a blood clot (corpus haemorrhagicum) which then forms the corpus
luteum. The granulosa cells enlarge, and become
vesicular, and are now called the granulosa lutein
cells. these become folded, as you can see here.
The spaces between the folds are filled with theca interna
cells, which also enlarge and become glandular,
and are now known as the theca lutein cells.
The zona granulosa cells begin to secrete progesterone
(granulosa lutein cells). The corpus luteum also secretes oestrogen
(which inhibits FSH) and relaxin (which relaxed the fibrocartilage
of the pubic symphysis).
If pregnancy does not occur, then the corpus luteum degenerates
into the corpus albicans, and levels of oestrogen
and progesterone fall, allowing release of FSH and LH.
If pregnancy does occur, then the syncytiotrophoblasts of the placenta
release human chorionic gonadotrophin, and the
corpus luteum persists.
About 20 primordial follicles start developing in each cycle, but
only ONE makes it!
This image shows a corpus luteum in a human ovary. (from anatomy.iupui.edu)
It takes up one third of the ovary.
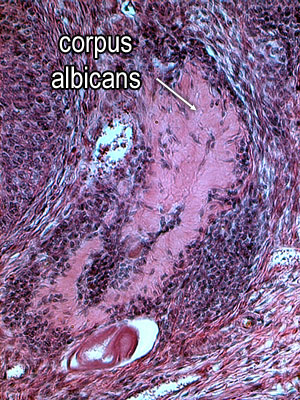
Corpus albicans
This image shows an atretic corpus luteum or corpus albicans.
The cellular elements have degenerated, and macrophages phagocytose
the dead cells. Fibrous tissue is left behind. The corpus albicans
looks pale. It will continue to shrink, eventually forming a small
scar on the side of the ovary.



